A friend or family member may have been recommended to consider shoulder replacement; maybe it has been recommended to you! All of a sudden, questions pile up in your mind: How painful is it? What’s the recovery like? Could I have complications? Will I have restrictions? How long do these implants last? You will be comforted to learn that, at least in my practice, many of these concerns are actually not that worrisome…
Why do we use the term anatomic shoulder arthroplasty?
The shoulder joint is formed by the round upper portion of the bone in the arm (humeral head) and the shoulder blade socket (glenoid). When joint damage results in severe pain, loss of motion, and functional limitations, shoulder replacement becomes the best solution for many. The closest we can get to “normal” when replacing the shoulder joint is by using artificial parts that are shaped to imitate the normal geometry of the shoulder: in an anatomic replacement, the humeral head is replaced with a metallic hemisphere, and the socket receives a new plastic surface. Another style of replacement called reverse, has been discussed in our blog before. Anatomic shoulder replacement is most commonly performed by separating the deltoid and pectoralis muscles and dividing one tendon (the subscapularis) to access the joint.
Pain control has been optimized so much!
If you know people that have undergone rotator cuff repair surgery in the past, they may have terrified you with horror pain stories. Luckily, we have learned a few tricks that tremendously help with pain control after shoulder replacement. Buzz words you will hear if you talk to your doctor include “block”, “long-acting local anesthetics”, “preemptive”, and “multimodal”. Confusing, huh?
Blocks. Pain and feeling are transmitted to the brain through a bundle of nerves, the brachial plexus. This transmission can be temporarily blocked by injecting a local anesthetic around these nerves. The block may last more than 12 hours with certain long-acting local anesthetics. The block will last even longer if a thin catheter is temporarily inserted around these nerves, to allow continuous delivery of local anesthetics. If the block is successful, there is no pain right after surgery; amazing! However, some individuals are bothered by the lack of feeling in the hand or the associated tingling.

Injecting the joint. Alternatively, the joint space may be injected with a large volume of long-acting local anesthetic, oftentimes combined with other medications such as steroids or opioids. Feeling in the rest of the arm is preserved, but sometimes these injections are not as effective as a block.
What does preemptive mean? Under general anesthesia, without a block or pain medication on board, the brain subconsciously receives pain signals as soon as the incision or skin cut is performed. These signals activate brain mechanisms that eventually lead to a worse pain experience. “Preemptive” means ensuring that pain transmission to the brain is minimized with medication or completely blocked by a local anesthetic before surgery starts. This leads to a much less painful experience. Hence, my preference is to provide my patients with a block and pain medication before going to the operating room. By the time surgery starts, the brain does not even know it!
What does multimodal mean? Pharmaceutical companies manufacture pain medications that work through different mechanisms. Each of these medications can be administered at increasing doses. Higher doses provide more pain relief, but doses can only be increased so much before side effects occur. Interestingly, combining multiple pain medications that work through different mechanisms seems to result in better pain relief than what you would expect if their individual effects were just mathematically added: 1 + 1 + 1 medications ends up helping more than 3! They enhance the efficacy of one another. “Multimodal” means using multiple pain medications that enhance each other in low dosages to reduce side effects. Preemptive multimodal analgesia combined with blocks or intraarticular injections makes shoulder arthroplasty a surprisingly comfortable experience.
What’s the recovery like?
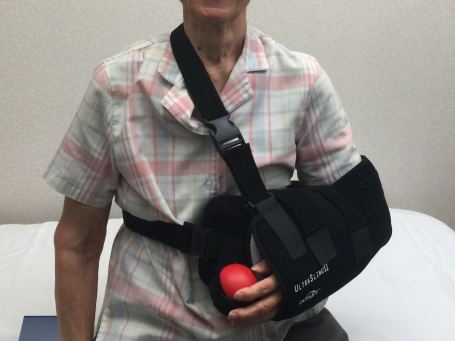
Most surgeons recommend use of a shoulder immobilizer for the first six weeks after anatomic shoulder arthroplasty. The idea is to protect the shoulder and avoid actively moving it. The only reason being is the need to protect the subscapularis tendon until it heals (remember, this is the only tendon divided in the operation). Therapy starts soon after surgery and progresses in three sequential phases: (1) passive motion, (2) active-assisted motion with stretching, and (3) strengthening. During the first 4-6 weeks, someone else (a friend, family member or physical therapist) gently moves the shoulder so that it does not freeze up. Once the subscapularis is healed, motion can be active (with assistance if needed), and the shoulder can be safely stretched. At week 10 to 12, strengthening starts, eventually incorporated elastic resistance bands. Although pain subsides very quickly after anatomic shoulder replacement, many patients do not feel their best, shoulder-wise, for a whole year!
Could I have complications?
Yes…, complications can happen after any surgery. The most worrisome complications include infection, nerve injury, failure of the subscapularis to heal, stiffness and instability. Luckily these complications are not very common. In the long term, the main problems are late tears of the rotator cuff (the replaced shoulder does not change the natural history of tendon disease) and loosening or wear of the implants.
Coping with restrictions to make your implants last
Shoulder replacement parts are mechanical and as such they can wear out or loosen up over time. Of the two replacement parts, the socket (glenoid component) is at greater risk (the humeral component rarely loosens). The shoulder bony socket is small to begin with, so the replacement part that can be fitted in the socket is small as well, and typically made of plastic, not metal. Multiple cycles of motion can eventually wear out or loosen this plastic implant. The key to make your implants last as long as possible is to understand what’s safe and what’s not.

Shoulder wear occurs as the metal ball moves on the plastic socket under excessive load. If you need to carry a heavy object after surgery, you can do it safely: bend your knees a little so that you can grab the object with your arm at your side, and carry it; since the shoulder never moved, little or no wear occurs. On the contrary, if you lift a very heavy object to a high shelf, for example, as the humeral ball glides on the socket, the whole weight of the object multiplies the load that the shoulder joint sees.
In my practice, after anatomic shoulder replacement I recommend individuals to avoid heavy lifting overhead with the affected side. Similarly, doing push-ups or weight training with exercises that require shoulder movement are not recommended: military press, bench pressing and lat dorsi weight training should probably be avoided, whereas biceps, triceps and traps are probably ok.
If you want to learn more…
One thought on “Answers to Common Questions About Anatomic Total Shoulder Replacement: The Patient’s Perspective”
Comments are closed.